Discover how to perform everyday tasks using MyMedicare.gov, the official Medicare online user portal, including opening an account, logging in and using the Blue Button.
Read moreSpeak with a licensed insurance agent
Speak with a licensed insurance agent
Compare plans today.
If you're approaching retirement, you may have questions about how this will affect your Medicare coverage. We can help!
Most people become eligible for Medicare at age 65, which is also the age at which many people retire. However, many American seniors are postponing retirement to continue working, and some are retiring early.
If you’ve retired or are approaching retirement age, you may have questions about how this will affect your Medicare coverage.
Below, we take a look at several scenarios to help you better understand your health insurance options whether you retire early, retire at 65, or continue working past the age of 65.
In most cases, you cannot sign up for Medicare before you turn 65, even if you retire early.
If you have health insurance through your employer’s group health insurance plan, we recommend finding out whether you will lose those benefits when you retire.
Some companies allow employees to remain on their employer-provided health insurance plan after they retire, and some do not.
If you retire earlier than age 65 and lose your group health insurance coverage, you may consider enrolling in a private health insurance plan until you are eligible for Medicare.
Once you are enrolled in Medicare, you can drop your private insurance coverage.
You’ll likely be automatically enrolled in Original Medicare three months before your 65th birthday if you’re already receiving Social Security or Railroad Retirement Board retirement benefits at least 4 months before you turn 65.
If you aren’t automatically enrolled in Original Medicare, you must manually enroll. The best time to manually enroll in Medicare is during your Medicare Initial Enrollment Period.
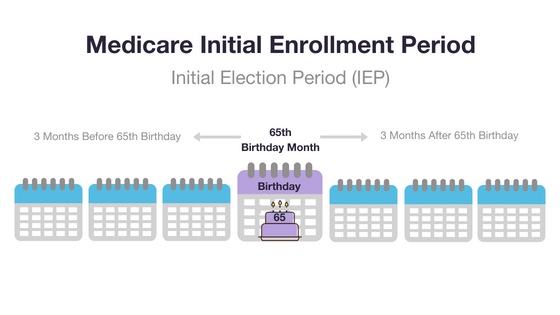
Typically, your Initial Enrollment Period begins three months before your 65th birthday, includes your birthday month, and ends three months after your 65th birthday.
Failure to sign up for Medicare during your Initial Enrollment Period could cause you to pay late enrollment penalties, resulting in permanently higher monthly premiums (unless you qualify for a Special Enrollment Period).
You can manually enroll in Original Medicare by:
Some people may qualify for Medicare before the age of 65 if they are receiving disability benefits from Social Security or the Railroad Retirement Board or have a qualifying medical condition such as ESRD.
If you continue working once you turn 65, you may have the option to keep your group health insurance plan until you retire.
We recommend speaking to your company’s human resources department or benefits manager to learn how your company handles group health insurance for people over the age of 65.
Most people do not pay a premium for Medicare Part A, as long as they paid sufficient Medicare taxes while working.
If you’re enrolled in premium-free Part A and are still on your employer’s group plan, your Part A coverage will not affect your group health insurance coverage, and you won’t have to pay a premium for your Part A benefits.
Unlike premium-free Part A, Medicare Part B requires you to pay a monthly premium for your Part B benefits ($202.90 per month in 2026, though it could potentially be higher based on your income).
If you’re still receiving health insurance benefits through your employer and are automatically enrolled in Medicare Part B, you may have the option to opt out of Part B until you retire or lose your group health insurance coverage.
Opting out of Part B will prevent you from having to pay monthly premiums for coverage you aren’t using. Once you retire, you should qualify for a Medicare Special Enrollment Period, which allows you to enroll in Part B later without facing a late enrollment penalty in most cases.
Special Enrollment Periods are times outside of your Medicare Initial Enrollment Period and the Medicare General Enrollment Period during which you can enroll in Medicare or make changes to your Medicare coverage.
If you’re still receiving health insurance through your employer, a Special Enrollment Period allows you to delay enrolling in Medicare Part B and Medicare Part D without incurring late enrollment penalties in most cases.
In order to qualify for a Special Enrollment Period, you must get confirmation of creditable coverage from your employer.
Typically, your Special Enrollment Period lasts for eight months and begins when your group coverage ends.
Medicare Part C (Medicare Advantage) is an alternative to Original Medicare that is available to most Medicare beneficiaries.
Medicare Advantage plans must provide at least the same benefits as Medicare Part A and Part B, and many provide additional benefits.
Before you can enroll in Medicare Advantage, you must enroll in Original Medicare (Medicare Part A and Part B).
If you’re still receiving health insurance benefits through your employer, you can keep your Part A coverage, drop your Part B coverage while you’re still insured by your employer, and then re-enroll in Part B once you retire.
If you’re ready to explore your Medicare Advantage options now, a licensed insurance agent can help you find MA plans in your area and get you enrolled in one that works for you.
Medicare Part D (Medicare Prescription Drug Plans) helps cover prescription drug costs, which is not a benefit offered by Original Medicare.
Medicare Part D requires you to pay a monthly premium in addition to your Part B premium.
If you do not enroll in a Part D plan when you’re first eligible and do not have confirmation of creditable coverage, you may have to pay late enrollment penalties if you decide to enroll in a Part D plan later.
If you have another source of creditable drug coverage (like a group health insurance plan that covers prescription drugs through your employer) you can choose not to enroll in a Medicare Prescription Drug Plan and will not face late enrollment penalties if you decide to enroll in a Medicare drug plan once you retire.
You can compare Part D plans available where you live and enroll in a Medicare prescription drug plan online when you visit MyRxPlans.com.
When you have Medicare and another type of insurance, one will be the primary payer and one will be the secondary payer.
Primary insurance pays first for your medical bills, and secondary insurance pays after your primary insurance.
Typically, the primary payer pays up to the limits of its coverage and the secondary payer only pays if there are costs the primary insurer didn’t cover. The secondary payer may not always pay all the uncovered costs.
If you have questions about whether Medicare is the primary or secondary payer in your situation, call the Benefits Coordination & Recovery Center at 1-855-798-2627 (TTY: 1-855-797-2627).
When it comes to keeping your group health insurance coverage after the age of 65, you have specific rights and protections under the law.
If you work for a company with more than 20 people, your employer cannot:
If you work for a company with fewer than 20 people, your employer may require you to enroll in Medicare Part B at the age of 65. We recommend speaking with your employer directly to learn more about your health insurance options when working past age 65.
Whether you’re retired or are planning to retire, a licensed insurance agent can help you better understand your Medicare options. Call today to speak with a licensed insurance agent.

Christian Worstell is a senior Medicare and health insurance writer with MedicareAdvantage.com. He is also a licensed health insurance agent. Christian is well-known in the insurance industry for the thousands of educational articles he’s written, helping Americans better understand their health insurance and Medicare coverage.
..Christian Worstell is a senior Medicare and health insurance writer with MedicareAdvantage.com. He is also a licensed health insurance agent. Christian is well-known in the insurance industry for the thousands of educational articles he’s written, helping Americans better understand their health insurance and Medicare coverage.
Christian’s work as a Medicare expert has appeared in several top-tier and trade news outlets including Forbes, MarketWatch, WebMD and Yahoo! Finance.
Christian has written hundreds of articles for MedicareAvantage.com that teach Medicare beneficiaries the best practices for navigating Medicare. His articles are read by thousands of older Americans each month. By better understanding their health care coverage, readers may hopefully learn how to limit their out-of-pocket Medicare spending and access quality medical care.
Christian’s passion for his role stems from his desire to make a difference in the senior community. He strongly believes that the more beneficiaries know about their Medicare coverage, the better their overall health and wellness is as a result.
A current resident of Raleigh, Christian is a graduate of Shippensburg University with a bachelor’s degree in journalism.
If you’re a member of the media looking to connect with Christian, please don’t hesitate to email our public relations team at Mike@tzhealthmedia.com.